 
Objective refers to the hard data you collect regarding the patient. It can also refer to things a patient’s family members tell you.  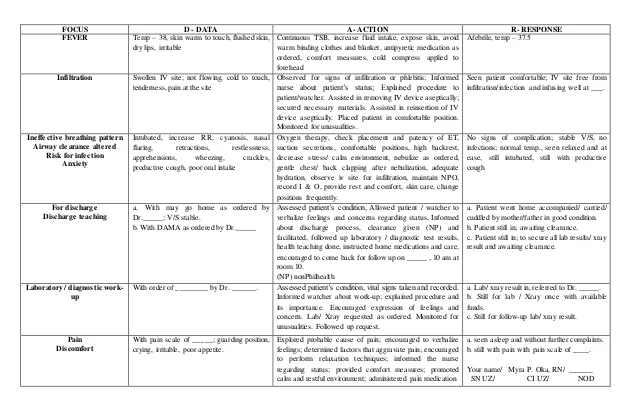
Subjective refers to things the patient can tell you, often including pain level and feelings or concerns. These are Subjective, Objective, Assessment, Plan, and Interventions. The term “SOAPI” is an abbreviation of the parts of the note. As always, check with your organization to determine how they want their notes written. This article will break the SOAPI note down so you can decide if it’s a format that will work for you. There are several different ways to write a nursing note, but this article will focus on one of the most popular and how it is written: the SOAPI note. Regardless, writing a good note at the end of your shift is essential for every patient. Most hospitals have gone to a computerized documentation system, but you may occasionally come across an institution that still does things with pen and paper. Some organizations have certain requirements for how charting must occur. Not only does charting provide nurses and doctors caring for a patient on future shifts an accurate picture of what happened on previous shifts, but it also becomes a permanent part of the patient’s medical record. While time-consuming, good charting is essential to providing top-notch patient care. You may have heard the adage in nursing school or from a co-worker: As a nurse, “if you didn’t chart it, it didn’t happen!” Charting takes up a large portion of your shift, especially if you do it correctly. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
